IBS and Systemic Nickel Allergy: The Connection Your Doctor Missed
IBS and Systemic Nickel Allergy: The Connection Your Doctor Missed
If you've been diagnosed with IBS and nothing seems to work — or if the low FODMAP diet only partially helped before your symptoms came back — there's something nobody told you.
Up to 30% of IBS patients may actually have a systemic nickel allergy driving their symptoms. And a low nickel diet may succeed where FODMAP failed.
Why IBS and SNAS Look Identical
The gastrointestinal symptoms of IBS and Systemic Nickel Allergy Syndrome are virtually indistinguishable. Both present with bloating, abdominal pain, diarrhea, constipation, nausea, and heartburn (Rizzi et al., 2017).
Both show up as "functional" GI disorders — meaning your colonoscopy looks normal, your blood work looks normal, and your doctor shrugs and says it's probably stress. Without specifically testing for nickel, there is no way to tell them apart clinically.
And studies consistently show that IBS patients have substantially higher rates of nickel sensitization than healthy controls (Rizzi et al., 2017).
What Nickel Actually Does to Your Gut
This isn't just "sensitivity." When a nickel-allergic person ingests nickel through food, it triggers a condition called Allergic Contact Mucositis (ACM) — localized inflammation in the gut lining (Picarelli et al., 2021).
Here's the cascade: Nickel activates TLR4 "danger sensors," triggering a low-grade immune response. This stimulates intestinal mast cells to release histamine and tryptase. And under electron microscopy, researchers have actually seen nickel physically widen the tight junctions between intestinal cells — confirming the "leaky gut" that many IBS patients suspect but can't prove (Miglietta et al., 2021).
That's real, measurable, structural damage. Not just "sensitivity." Not just stress.
The Clinical Evidence
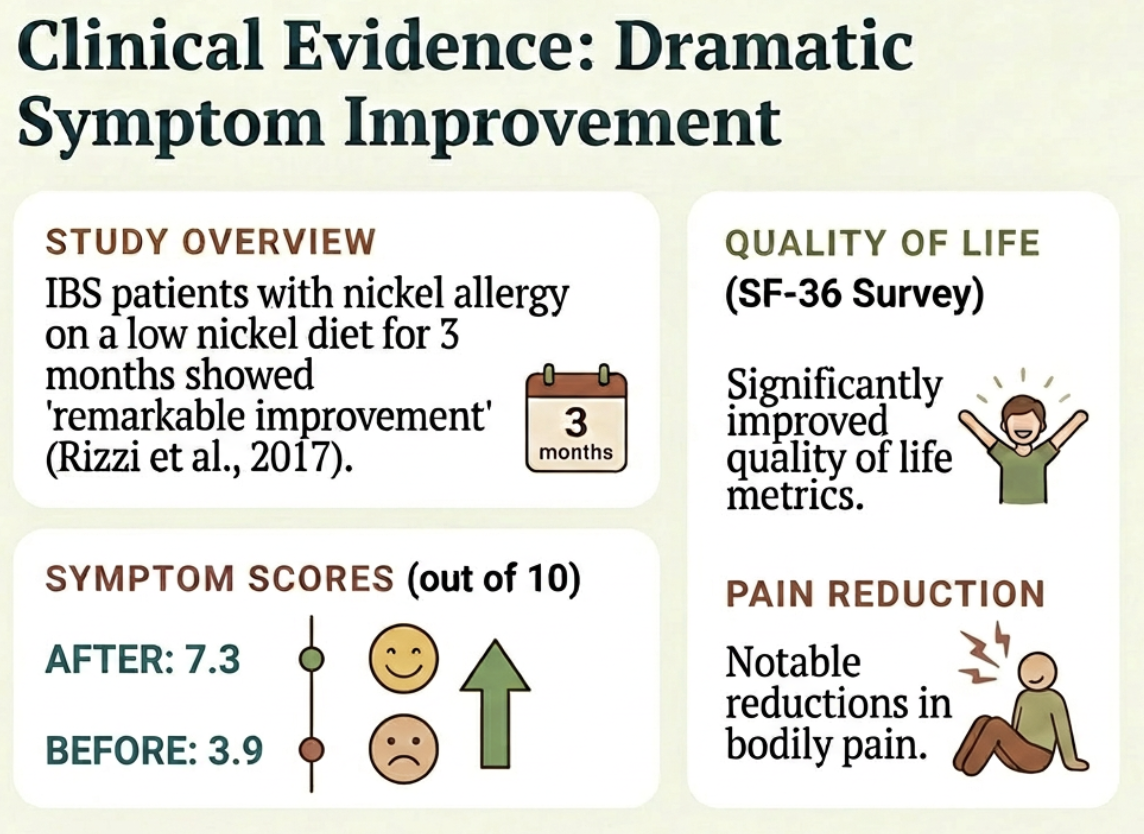
In a prospective study of IBS patients with confirmed nickel allergy, following a low nickel diet for three months resulted in what researchers called a "remarkable improvement" in almost all gastrointestinal symptoms (Rizzi et al., 2017).
The numbers: symptom improvement scores jumped from 3.9 to 7.3 out of 10. Quality of life scores improved significantly, especially in the reduction of bodily pain. And the diet also improved intestinal permeability — helping to heal the physical damage to the gut barrier.
For patients with gut-based nickel allergy diagnosed via the oral mucosa patch test, 98.1% saw improvement in just two months on a low nickel diet (Picarelli et al., 2010).
Why Low FODMAP Only Partially Works
If the low FODMAP diet sort of worked for you but then you plateaued or relapsed, this is likely why.
The low FODMAP diet restricts fermentable carbohydrates. The low nickel diet restricts a metal. But there's massive overlap in restricted foods — both diets cut beans, legumes, and certain vegetables (Borghini et al., 2020).
When you went low FODMAP, you accidentally removed some high-nickel foods. That's why you felt partially better. But FODMAP also allows many high-nickel foods — like oats, chocolate, and nuts. The nickel never fully left your plate.
Patients who "fail" the FODMAP diet often respond to the low nickel diet because they were targeting carbohydrates when their actual trigger was the metal all along.
The "Healthy Diet" Trap
If your IBS started or worsened when you switched to a "healthy" plant-based diet, you're not crazy. Whole wheat, oats, legumes, soy, nuts, and spinach are all nickel hyper-accumulators (Picarelli et al., 2021). Your gut-healing diet was flooding your gut with the exact allergen causing the inflammation.
The Gluten-Free Relapse
Many IBS patients go gluten-free, feel better initially, then watch their symptoms return aggressively months later. Here's why: you felt better because you stopped eating wheat, which is high in nickel. But the main substitutes in a gluten-free diet — corn and soy — are also hyper-accumulators of nickel (Picarelli et al., 2021; Borghini et al., 2020).
You didn't fail the diet. The diet swapped one nickel source for another.
Your Next Step
If you have IBS and this resonates, the first step is understanding which foods are high in nickel. Download my free Nickel Food List to see exactly what's in your current diet.
Download the Free Nickel Food List →
Next in the series: why your acid reflux might actually be a nickel allergy — and why your PPI isn't fixing it.
References
Borghini R, Porpora MG, Casale R, Marino M, et al. Irritable Bowel Syndrome-Like Disorders in Endometriosis: Prevalence of Nickel Sensitivity and Effects of a Low-Nickel Diet. An Open-Label Pilot Study. Nutrients. 2020;12(2):341.
Calogiuri GF, Bonamonte D, Foti C, Al-Sowaidi S. Nickel Hypersensitivity: A General Review on Clinical Aspects and Potential Co-Morbidities. J Allergy Ther. 2016;7(5):243.
Greco N, Pisano A, Mezzatesta L, et al. New Insights and Evidence on "Food Intolerances": Non-Celiac Gluten Sensitivity and Nickel Allergic Contact Mucositis. Nutrients. 2023;15(10):2353.
Miglietta S, Borghini R, Relucenti M, et al. New Insights into Intestinal Permeability in Irritable Bowel Syndrome-Like Disorders: Histological and Ultrastructural Findings of Duodenal Biopsies. Cells. 2021;10(10):2593.
Picarelli A, Di Tola M, Vallecoccia A, et al. Oral Mucosa Patch Test: A New Tool to Recognize and Study the Adverse Effects of Dietary Nickel Exposure. Biol Trace Elem Res. 2010;139(2):151-159.
Picarelli A, Greco N, Sciuttini F, Marini C, Meacci A. High consumption of Nickel-containing foods and IBS-like disorders: late events in a gluten-free diet. Ecotoxicol Environ Saf. 2021;222:112492.
Rizzi A, Nucera E, Laterza L, et al. Irritable Bowel Syndrome and Nickel Allergy: What Is the Role of the Low Nickel Diet? J Neurogastroenterol Motil. 2017;23(1):101-108.